Tachypnoea similarly increases the child’s fluid requirement two- to three-fold. Water is required to facilitate this heat exchange, which increases the day-to-day water requirement for the child as compared with the adultįor example, a fever above 38˚C requires an increase in the child’s fluid intake of 10–12% because of the increased radiant heath, and thus water, loss. The high metabolic rate in the child means an increased energy expenditure, including thermal energy, thus a high rate of heat exchange. Children therefore have a higher metabolic rate than adults, which in turn means that they proportionately require more water for both intercellular and intracellular synthesis and excretion of metabolic wastesĬhildren have a high rate of heat exchange

The concept thus adds to the child’s increased biological need for waterĬhildren are highly metabolic individuals because of their ongoing growth and development, as well as their other life activities.
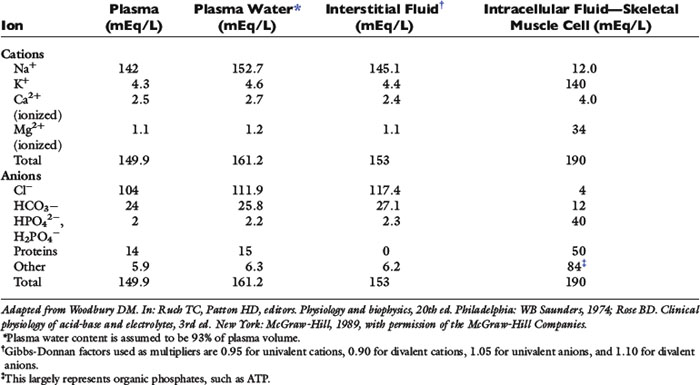
Electrolyte composition of body fluid compartments skin#
This increases water loss from the child through the skin in heat loss by radiation to the environment. The surface area-to-volume ratio of a small child is greater than that of an adult. The close encounter of ECF with the environment thus means a higher turnover rate of ECF in the child than the adultĬhildren have a large surface area-to-volume ratio meaning a higher insensible fluid loss from the skin and airways perfusing the subcutaneous capillaries underneath the skin. Higher ratio of extracellular fluid volume to that of intracellular fluid volumeīlood plasma forms part of the ECF and it is this body fluid that is in direct contact with the environment, e.g. Table 25.3 Why children need more water than adults The only saving grace in preventing adverse outcomes in these circumstances is the careful monitoring of serum sodium levels in the children ( Au et al 2008). There is increasing evidence to show that iatrogenic (treatment – induced) hyponatraemia is a real clinical threat to children especially in the postoperative period and the high-dependency setting. Unrelieved, cerebral neuropathy resulting from the increased ICP can cause seizures, coma and death. Cerebral function is altered, and this is reflected in an abnormal score on the Glasgow Coma Scale. Ultimately, cytotoxic cerebral oedema, with its attendant raised intracranial pressure (ICP), occurs. Here, the cells most vulnerable to osmotic fluid shift into their intracellular compartment are brain cells. A similar situation will occur in water intoxication or overhydration with acute hyponatraemia. Water will then move by the process of osmosis into the erythrocytes, causing them to swell until their cell membrane can no longer accommodate the increase in cell volume, causing them to burst (cell lysis). erythrocytes) to exist in a hypotonic environment relative to their intracellular space. Theoretical intravenous administration of pure water causes the cells (e.g.
Daily fluid maintenance requirements take into consideration losses from the skin, airways, gastrointestinal tract and urine. For a thorough comprehension of the value of water to life, growth and development, and hence the deleterious effects of uncorrected body fluid and electrolyte imbalance, an understanding of the chemical and physical properties of water is essential (see Chapter 27 in Martini Nath, 2009). A healthy adult can survive for around 10 days without water a healthy child will survive only 3–4 days without water.
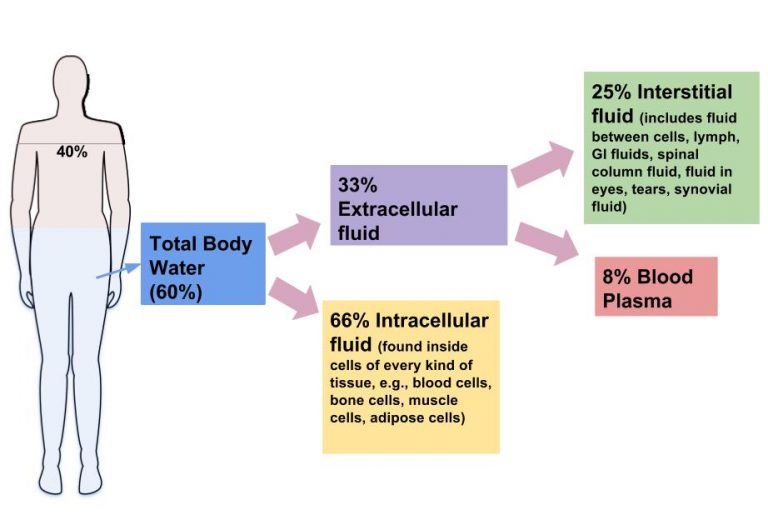
In the absence of water, chemical reactions, metabolic processes and regulatory systems become severely compromised and eventually cease to function (Tortora & Derrickson 2009). Table 25.1 shows the water composition of various tissues in the average individual. Two-thirds of the total body weight is water and it is the body’s single most important constituent ( Martini & Nath, 2009). Water is vital to the existence of all living organisms and is the most abundant molecule of their cell mass ( Campbell & Reece 2008).
